If you’ve been experiencing breakouts that just don’t seem to respond to the many different acne treatments out there, then it could be because those bumps aren’t actually acne.
Enter fungal acne; the imposter condition that looks just like regular acne, feels just like typical acne, but is actually completely different. This may sound confusing, but this article will clear everything up for you – here’s all you need to know when it comes to identifying, treating, and preventing fungal acne.
Contents
Is Fungal Acne a Real Thing?
Fungal acne is very much a real thing. However, it’s true that its name is contradictory since true acne, otherwise known as acne vulgaris, cannot actually be caused by fungus, only by bacteria. Instead, fungal acne is a colloquial term for a skin condition technically known as pityrosporum folliculitis or malassezia folliculitis.
What Causes Malassezia Folliculitis?
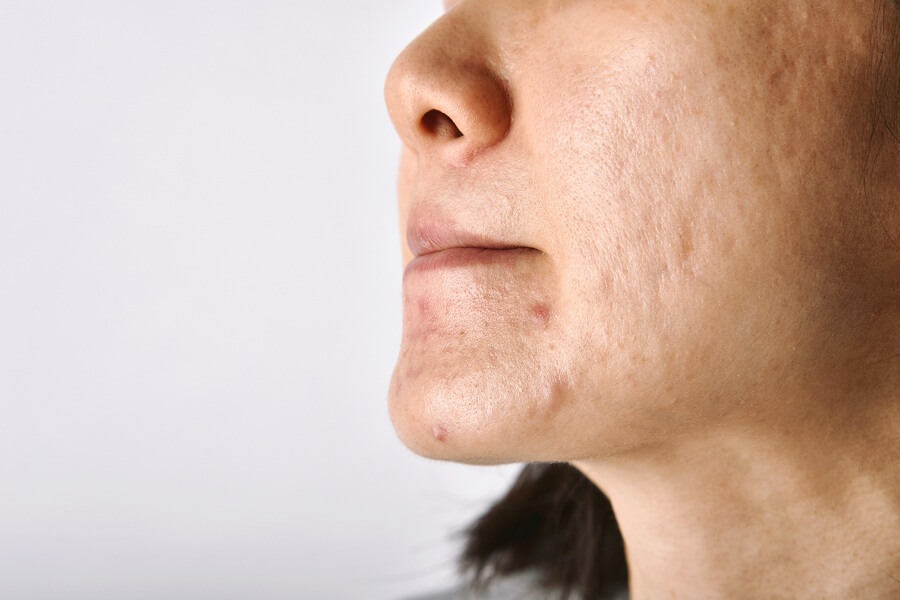
Malassezia folliculitis (MF) is named after a specific type of yeast, which is classed as a fungus. While it’s completely normal for this yeast to be living on your skin, certain factors can lead to an overgrowth of yeast. This results in infection in the hair follicles in your skin, with those small, pimple-like bumps that appear known as malassezia.
Some of the main causes that trigger this yeast overgrowth, and therefore fungal acne breakouts, are:
- Sweat
- Humidity and heat, making problems more prevalent during the summer months
- Tight clothing
- Overuse of antibiotics and other medications, since these interfere with your skin’s natural yeast balance
- Close contact with someone else who has fungal acne, since yeast is prone to spreading
- Health conditions that weaken the immune system, such as diabetes or HIV
- Genetics
- Certain beauty products
Is Your Acne Fungal or Bacterial?
Market research shows that people often struggle to differentiate between fungal acne and regular acne, so here’s how to tell which one you’re dealing with. While acne vulgaris usually manifests as a variety of different whiteheads and blackheads, each a slightly different size, MF looks more consistent and uniform. You’ll notice red bumps on your skin, and sometimes also whiteheads and blackheads too, but these will all be around 1mm in size.
Although pityrosporum folliculitis does sometimes affect the face, breakouts are usually most prevalent on the upper body. Another common symptom is bumps that feel itchy, which doesn’t happen with the regular type of acne.
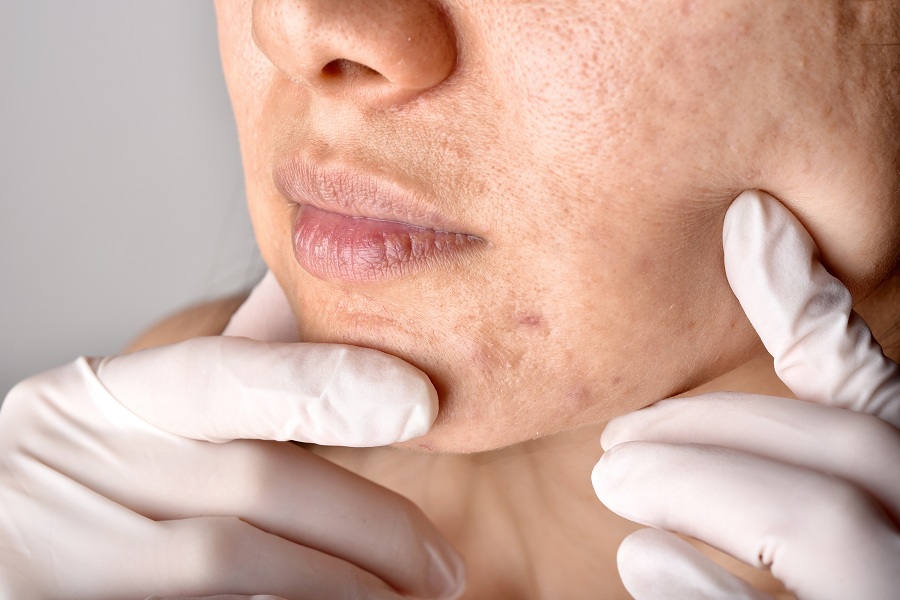
How to Treat Fungal Acne
Since fungal acne and regular acne are two completely different skin conditions, it’s not surprising that traditional acne treatment products don’t have an effect on malassezia. Instead, look into the following:
Wash Away Fungal Acne with a Dandruff Shampoo
This may sound a little strange at first, but it’s one of a few off-label tricks that even the best board-certified dermatologist out there would recommend.
Dandruff shampoos, such as Selsun Blue or Head and Shoulders, usually contain either pyrithione zinc or selenium sulfide as an active ingredient. Both are extremely effective at treating MF, which is why those suffering from it will often use a dandruff shampoo as a body wash (provided your spots are on your body, rather than your face).
Apply the shampoo to your body and then leave it to sit on your skin for a few minutes. This gives the ingredients within some extra time to work. Then, rinse it off and repeat regularly throughout the week.
Start Using an Over-the-Counter Treatment
There isn’t a huge choice when it comes to over-the-counter creams for fungal acne, although constant product development means that this could soon change. But, again, there are effective products available that can be used off-label. The best are the creams and ointments that have been designed for athlete’s foot or jock itch, but make sure that they contain one of the following ingredients:

- Ketoconazole
- Butenafine
- Clotrimazole
Dermatologist-Approved Home Remedies for Fungal Acne
There are a few home beauty remedies out there that have proven to be effective at eliminating excess yeast in hair follicles.
The first is tea tree oil, which naturally has antifungal and antiseptic properties. Dilute a couple of drops of tea tree with a carrier oil before applying this to the bumps on your skin. However, since tea tree oil is known for its potentially irritating side effects on sensitive skin, do a patch test first to make sure that your skin can tolerate it.
Honey, witch hazel, apple cider vinegar, and turmeric all also have antifungal and antimicrobial properties. Just like tea tree oil, these can be applied directly to problem areas. Do this regularly and consistently for maximum benefits.
Visit Your Dermatologist for an Oral or Topical Treatment
If all of the above fails, then it’s time to turn to a board-certified dermatologist, or even your regular doctor, for some extra help. Depending on your symptoms, your dermatologist will either recommend an oral antifungal medicine or a topical treatment.
Prescription treatments are designed to directly target the yeast in each hair follicle, meaning that they’re much more effective and faster-acting than standard creams and ointments.
How to Prevent Fungal Acne

Once any existing breakouts are under control, it’s time to turn your attention to prevention techniques. Here’s what you need to do to make sure that fungal acne doesn’t cause anymore problems in the future:
Wear Loose and Breathable Clothes
If you frequently wear tight clothes, especially when you’re doing anything that leads to your body sweating, then this is one way to cut back on breakouts. Tight, sweaty, and damp clothes provide the perfect environment for yeast overgrowth, which will soon result in an MF breakout. Instead, swap any restrictive clothes for looser and more breathable alternatives.
Shower When Sweaty
If you sweat quite often, then try increasing how often you shower. Leaving sweat to settle into your skin cells and each hair follicle will not only lead to inflammation and the regular type of acne, but it’ll also encourage fungus and yeast growth, causing fungal acne too.
Regularly Exfoliate

Exfoliation is something that everybody should be doing. However, if you’re dealing with fungal acne, then you really don’t want to end up skipping an exfoliation session.
The combination of dirt, oil, and dead skin cells is believed to contribute to fungal acne symptoms. Exfoliation is the best way to clear your pores of these unwanted substances, with chemical exfoliants being the most beneficial.
Use the Right Skincare Products
There are so many different beauty and skincare products out there, but some could actually worsen fungal acne. Take a look at the product information on any cosmetics that you use – everything should be non-comedogenic, meaning that their formulas don’t contain any pore-clogging ingredients.
This is something that those with regular acne need to do as well. Excess oil on your skin will lead to inflammation, which could then trigger fungus growth.
When it comes to the specific products that you need, a good moisturizer (non-comedogenic, of course) is a must. A brightening, anti-blemish serum that helps to reduce natural oil production would also be useful, as would a cleanser containing salicylic acid.
Eat a Healthy Diet
Carbohydrates feed yeast in the body, meaning that the more carbs you eat, the faster the natural yeast on your skin will multiply. Research information shows that cutting back on carbs can reverse this, so take a good look at what you’re eating if you really want to keep fungal acne at bay.
FAQs

Is fungal acne curable?
Yes, fungal acne is definitely curable, so long as you treat it correctly, instead of using treatments designed for regular acne.
What foods help with fungal acne?
The best foods for preventing fungal acne are those that are low in sugars, carbohydrates, and yeast. In terms of treating fungal acne through your diet, increase your consumption of probiotics and look into naturally antifungal foods, such as oregano and garlic.
Where does fungal acne appear on the face?
Fungal acne usually develops on the body, although the forehead tends to be particularly prone to it too. That being said, MF can occur just about anywhere on the face or body where hair follicles lie.
Conclusion
Due to how it looks so similar to regular acne, many people end up using the wrong treatments to deal with fungal acne, meaning that those bumps never actually go away.
However, this article has hopefully helped you to identify the condition and understand how it differs from standard acne. This means that you’ll now be able to take the best acne treatment and prevention steps in order to get the health of your skin back to normal as soon as possible.